Our CCM and BHI software expedites every step of the process, allowing you to efficiently capture and bill for your own CCM and BHI activities. We're committed to your success, and we'll be there as your teammate for all things CCM and BHI.
We provide a convenient consent outline that your team can use with patients.
With our built-in templates, your team can create care plans with ease.
Our time tracking tools help your team efficiently log CCM and BHI activities.
We make it easy to track the billing status of patients and generate reports.
With our platform, you can pursue CCM and BHI seamlessly. After all, we're designed by doctors for doctors.
We enable you to leverage your own care services to provide CCM and BHI in-house without any headaches.
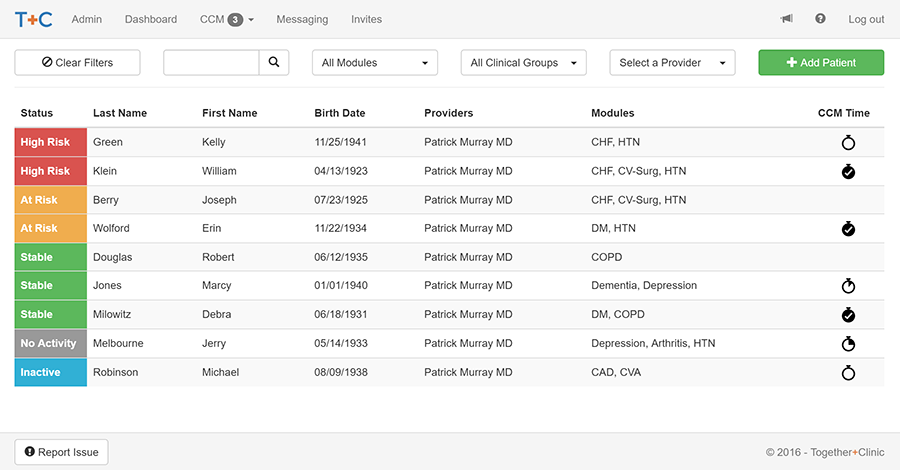
Crafted for clinical workflows, our software helps you efficiently track your CCM and BHI activities.
Our platform simplifies billing, helping you receive new reimbursements for your Medicare patients.
Want to learn more about Medicare's CCM program? Check out our CCM and BHI Survival Guide.
CCM (billable under CPT 99490) and BHI (billable under CPT 99484) presents a great way to improve patient connectivity and increase revenue through your own care services.
Note: Any care team members acting under general supervision of the provider can contribute.
Curious to learn more or get started? Please schedule a demo or give us a call at (800) 618-6990.